Introduction
Let’s talk about something real—Gynaecological cancers. You might hear those words and instantly feel a bit uneasy. These are cancers that can start in places like your ovaries, uterus, or cervix. They often sneak in quietly. Most times, you don’t even notice until things get serious. That’s why awareness matters so much.
Think about this: You wouldn’t ignore a strange noise in your car, right? You’d check it out before it became a big problem. The same goes for your body. When you know what signs to look for, you catch things earlier. I want you to know—early detection can mean the difference between a quick fix and a long, hard fight.
So, let’s break the silence, clear the confusion, and learn how to listen to our bodies—because you deserve to feel safe and strong.
Statistics
Let’s look at the numbers of Gynecological Cancers. They really tell a story. In India, cervical cancer is everywhere. It’s the second most common cancer for women here. Over 1.27 lakh new cases were reported last year. The numbers from 2020 and 2022 barely changed. That’s worrying.
This means, not much progress yet. The global mortality rate for cervical cancer is 7.1 per 100,000 women. But in India, it jumps to 11.2. That’s way higher. Too many women are dying. The cancer burden keeps rising. By 2025, experts predict almost 30 million cases in India. That’s huge.
Survival rates are tough. Only half of cervical cancer patients survive for five years. Breast cancer is doing a bit better. Still, every number is a mother, a sister, a daughter. Behind every statistic, there’s a family. There’s fear, hope, and heartbreak.
Most importantly, many Gynecological Cancers come from lifestyle risks. Change is possible. Awareness can save lives. That’s why this matters. That’s why we talk about it.
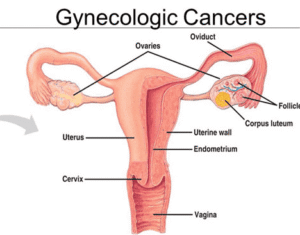
What are Gynaecological Cancers?
Let’s keep it simple.
Gynaecological cancers start in a woman’s reproductive organs. These include the uterus, ovaries, cervix, vagina, and vulva. They are different from other cancers.
Why?
They grow in places only women have. They need different tests. They show unique signs. You can’t compare them to lung or stomach cancer. Each one acts differently. Each one needs its own care.
Who is at risk?
Honestly, any woman can get these cancers. Age, family history, and infections matter a lot. Even lifestyle plays a part. If you have a close relative with cancer, your risk goes up.
If you’ve had certain infections, your risk is higher. You should know your own risk. You should talk to your doctor. Awareness helps you stay safe. Prevention starts with knowing the facts.

Types of Gynaecological Cancers
Let’s break them down.
First, there’s ovarian cancer.
It hides well. It often stays quiet until late. You may feel bloated or have tummy pain. Sometimes, you lose weight fast. Many women miss the early signs.
Next comes uterine cancer.
It grows in the womb. You may spot unusual bleeding. It often shows up after menopause. If you see blood after your periods stop, check with your doctor.
Cervical cancer is another big one.
It starts in the cervix. Often, it links to HPV infection. Regular Pap smears help find it early. You may notice bleeding after sex or between periods.
Vaginal cancer is rare. It starts inside the birth canal. You may notice discharge or pain. Sometimes, there’s a lump you can feel.
Vulvar cancer affects the outer parts. It can cause itching or burning. Sometimes, you see a sore that won’t heal.
Gestational trophoblastic tumours are very rare. They come from pregnancy tissue. You may get bleeding during or after pregnancy. They need special treatment.
Let me mention breast cancer. It’s not a gynaecological cancer. Still, it matters for women’s health. If you spot a lump in your breast, talk to your doctor. Always stay alert. Awareness saves lives.

Symptoms of Gynaecological Cancers
Let’s talk about symptoms of Gynecological Cancers. You may not notice them at first. They often start small. But you should know what to watch for.
Unusual bleeding is a big sign. Pain in your pelvis can mean trouble.
So can bloating that won’t go away. If you feel full quickly, take note of this. Unusual discharge matters too. If you see sores or lumps, don’t ignore them.
Even itching or burning can be a warning. Your body tells you when something’s wrong. You just have to listen.
Now, let’s get specific.
Ovarian cancer often brings bloating and belly pain. Uterine cancer usually means bleeding after menopause. Cervical cancer might cause bleeding after sex or between periods.
Vaginal cancer can show up as pain or a lump inside. Vulvar cancer may give you itching or sores that won’t heal. Gestational tumours might cause heavy bleeding in pregnancy.
Every cancer acts differently. Every sign matters. If you notice any of these, talk to your doctor. Early action saves lives. Always trust your gut.

Risk for Gynaecological Cancers
Let’s talk about risk. In Gynecological Cancers Family history matters a lot.
If your mother or sister had cancer, your risk is higher.
Lynch syndrome raises the risk even more. You should share your family history with your doctor.
Next, HPV infection is a big factor. It’s the main cause of cervical cancer. You can get HPV from sexual contact. Vaccines help protect you, but not everyone gets them.
Tamoxifen is a medicine for breast cancer. Sometimes it increases the risk of uterine cancer. If you use it, you need regular check-ups.
Chronic anovulation is another risk. If you have PCOS or you’re going through menopause, your periods can be irregular. Hormones get out of balance. Cancer risk goes up.
Nulliparity means never having been pregnant.
Infertility can add to your risk. Your body misses protective changes from pregnancy. Smoking, obesity, and age all count too. Early periods or late menopause stretch hormone exposure. That raises risk.
Your choices matter. Your body’s history matters. Knowing your risks gives you power. Always discuss these with your doctor. Prevention starts with awareness.

Gynecological Cancers screening tests for women:
Screening is your best defence from Gynecological Cancers. I always start with a pelvic exam. It helps spot lumps or changes early. The Pap smear is next. It looks for changes in your cervical cells.
FOGSI says start screening at 25 if possible. Or at 30 if resources are tight.

If your first test is normal, repeat every three years. That’s not too hard. High-risk HPV testing is also key. It finds the virus before cancer develops. This test can be done every 5–10 years if the results are good.
In some places, you may only get screened twice in your life.
Once at 35, then again at 45. But more is better when possible.
Screening usually stops at 65 only if you have three normal Pap smears or two negative HPV tests in ten years.
In low-resource areas, FOGSI suggests HPV testing or VIA every 3–5 years.
I also trust transvaginal sonography. It checks your uterus and ovaries. CA 125 is a blood test for ovarian cancer. It’s not perfect, but it helps.

An endometrial biopsy checks the lining of your womb.
Mammography is for breast cancer. It’s quick and saves lives.
Early detection changes everything. It gives you more options. It gives you hope. So, don’t skip your screening. Your health deserves it.

Treatment Options for Gynecological Cancers
Treatment looks different for everyone with Gynecological Cancers.
First, surgery is common. Doctors may remove the tumour. Sometimes they remove the whole organ. It depends on the stage. Surgery works best when cancer is found early.
Next, chemotherapy steps in. These are strong medicines that kill cancer cells. You may get them by drip or as pills. Chemo affects the whole body. It often comes with side effects. But it can save lives.

Radiation therapy is another choice. It uses high-energy rays to target cancer. Sometimes it’s used alone. Other times, it’s paired with surgery or chemo. It’s quick and focused.
Targeted therapy is newer. It attacks only cancer cells. Your healthy cells stay safe. Fewer side effects, more hope. Doctors use tests to see if this works for you.
Then, there’s immunotherapy. It helps your body fight cancer. It boosts your natural defences. Some women get great results. It’s not for everyone, so doctors check first.
Palliative care is special. It’s not just for the end. It helps you feel better during treatment. It eases pain, handles stress, and offers support. Every treatment plan is personal. Every step counts. You are never alone.

Prevention & Lifestyle Tips-
Let’s get real about prevention.
First, I always recommend the HPV vaccine. It protects you from the virus that causes most cervical cancers. It’s safe. It works best if you get it early. I wish every girl got this shot.
Oral contraceptive pills also help. They lower the risk of ovarian and uterine cancers. But talk to your doctor first. Every woman is different. What works for one may not work for another.
Breastfeeding has a bonus. It can protect you from some cancers. Even a few months helps. It’s good for babies and good for you.
Healthy habits matter most. Eat fresh food. Move your body every day. Get regular checkups. Find problems before they grow. I always say, prevention is power.
Smoking is a big risk in Gynecological Cancers. It hurts every part of your body. Quitting now helps you later. It’s tough, but it’s worth it.
Every small step counts. Start today. Stay strong. Prevention starts with you.
Conclusion
Let’s wrap this up. Gynaecological cancers are serious, but you have power. You can lower your risk. You can spot warning signs early. Think of it like caring for your car. You check the oil. You listen for strange sounds. You fix small problems before they grow. Your body deserves the same attention.
Screenings matter. Vaccines matter. Healthy choices matter. Even simple things help. Eat well. Move more. Quit smoking. Trust your gut if something feels off. Always ask your doctor questions. Share what you learn with friends and family.
Early action saves lives. You’re not alone. With knowledge and support, you stand strong. Take care of yourself. You’re worth it.
About the Author:
Dr Supriya Mahajan, M.S., D.N.B. (OBGY), is the Best Lady Gynecologist in Thane West. She has 10+ years of experience. She specialises in advanced laparoscopy, infertility, and high-risk pregnancy. She practices at Ova Fertility & woman Care & Currae Hospital in Thane.

